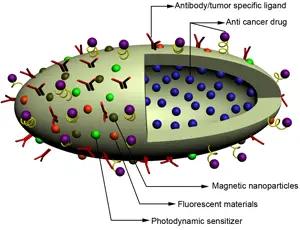
Gene therapy entails replacing an “abnormal” disease causing gene with a healthy, “normal” one. The method used for transfer of the gene into a target cell is via a carrier molecule called a vector, usually a virus that has been genetically altered to carry normal human DNA. Most viruses infect a cell by inserting their encapsulated genes into human cells in a pathogenic manner. By taking advantage of this mechanism and replacing the virus’ disease-causing genes with therapeutic genes, scientists have been able to precisely target treatment.
The herpes simplex virus type 1 protein, VP22, demonstrations the extraordinary property of intercellular transfer whereby proteins spread from their originating cell to numerous adjacent cells. This function of VP22 is being applied to overcome a major obstacle in gene therapy: proficient transfer of genes and gene products.
Polypeptides, consisting of VP22 fused to the tumor suppressor protein—p53 protein, have the ability to spread between cells and accumulate in recipient cell nuclei. This chimeric protein has been shown to effectively induce apoptosis (diseased cell death) in p53 negative human sarcoma cells, thereby inducing a pervasive cytotoxic effect.
The lack of functional p53 protein in the cell has been linked to more than 50% of all human cancers. The intercellular delivery of functional p53–VP22 fusion protein is likely to become an important therapeutic method of restoring cellular p53 function.
TFOT has previously reported on other cellular cancer treatments including the article “Smart Bombing Cancer with a Virus” describing how researchers at North Carolina State University have modified a common plant virus to deliver drugs specifically into cancer cells without harming the surrounding tissue. Another related TFOT story describes a new method to administer drugs targeted at cancer cells. To find out more about the treatment described in this article, please read the original study here.