Researchers at the University of Florida have discovered an enzymatic switch that allows some cells to live and leaves nearby cells to die. These results may be a key discovery in the fight against Alzheimer’s disease.
|
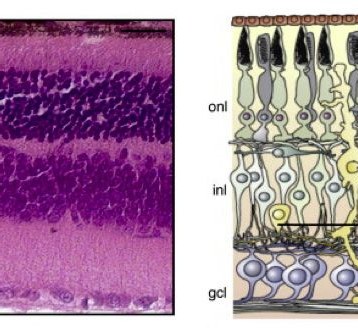
The hippocampus is an anatomical region of the brain which is shaped like a curved kidney bean in mammals. This structure is known to have an important role in the formation of memories and some function in motivation and emotions. Some parts of it are especially vulnerable to decreased cerebral blood flow, which can result from a stroke or circulation problems. The same vulnerable area is also one of the first regions to show pathology associated with Alzheimer’s disease.
The scientists from the McKnight Brain Institute at the University of Florida have researched rats’ cells in two nearby regions of the hippocampus. They have leaned that a recently discovered enzyme, PHLPP, pronounced “flip,” is probably acting as a silencer to a vital cell-survival protein in the region where neurons are most likely to be damaged and die.
AKT is a protein that upon activation hinders many naturally occurring inducers of cell death, thus ensuring the cell’s survival. The researchers studied the aforementioned regions for AKT presence and were not surprised to discover that AKT levels were lower in the cells that were more susceptible to damage and death.
The scientists wanted to understand what was causing the low levels of AKT. The research led the scientists to think of PHLPP1 – another recently discovered enzyme believed to be a natural tumor suppressor. Testing the hippocampal regions again they found that when PHLPP1 levels were high, the activation level of AKT was low. This corresponded with the more vulnerable cell areas.
Can this discovery be used to treat diseases resulting in hippocampal damage and memory loss, such is Alzheimer’s? “Possibly, we have found a target that could be manipulated with drugs so that these brain cells can be saved from threats,” said Tomas C. Foster, a professor of neuroscience at the University of Florida College of Medicine. “If one area of the hippocampus has a deficiency in cell-survival signaling, it is possible to find a way to ramp up the AKT protein. The caveat is, there are studies that show over-activating AKT may not be good for memory — AKT may be naturally lower in this region for an important reason. But in times of intense damage, there may be a therapeutic window to upregulate AKT and get some benefit to health.”
TFOT has recently covered the first clinical trial of Dimebon as a treatment for Alzheimer’s disease conducted by Medivation, San Francisco. We also covered several stories on the mechanism of memory creation, including a research conducted at the Weizmann Institute, in which scientists discovered an enzyme capable of erasing memories by disrupting the synapse maintenance and the story of a mechanism allowing for memory deletion, which was discovered at the Bristol University.
More information on the cell vulnerability switch can be found in the University of Florida news page.